Persisting Symptoms
Physiotherapy is a suitable treatment method for many musculoskeletal disorders. On the following page you will receive further information on the most common disorders that are treated in our practice. The information provided is short and precise, in order to provide a general overview. It does not replace a thorough medical examination. For questions regarding the described disorders or other symptoms please contact our therapists who are happy to help.
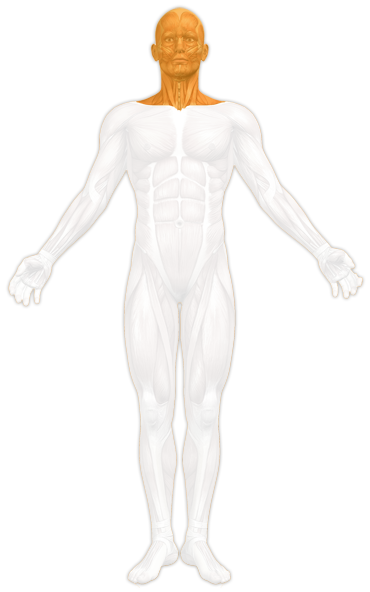
Head, neck and jaw
False posture, incorrect straining at work and persisting high stress levels can cause muscle tenseness around the cervical spine, a tension headache or also jaw joint discomfort. If there is pain radiating into the arms, further diagnosis is necessary so that a possible herniated disc can be diagnosed.
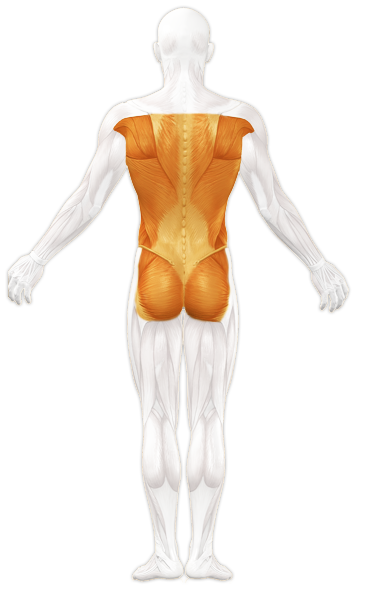
Back
Back pain is common in modern society. 80% of all adults experience at least one episode of back pain during their life. Often this pain disappears on its own after a short time. However, if it does not subside after a longer period of time, the cause of discomfort should be pinpointed, which is often connected to the musculoskeletal area. Yet, the pain can also result from stress or become intensified. Aside of this usually non-dangerous and yet bothersome, nonspecific back pain, structural changes such as a herniated disc, spinal stenosis or spondylolisthesis can occur. Such alterations need further clarification.
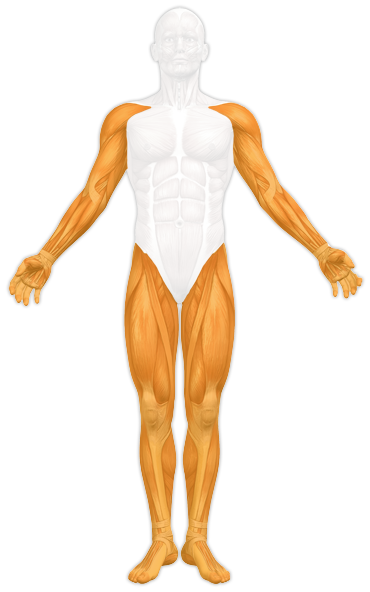
Arms and Legs
Especially during intense, athletic pressure the joints are highly strained. A cruciate rupture, a tennis elbow, a supination trauma or tears in the rotor cuff can be the result. Prevention aims to stabilize joints in a way that such harm cannot occur. Following an injury, the therapy must be adjusted to the process of healing so that full resilience can be regained. An arthrosis, which is a sign of wear and tear of the cartilage, can develop after years of high strain. In this case, the therapeutic emphasis lies on movement, posture and reducing pain.
Headache and migraine
Almost half of the population suffers from a headache at least once a year. Its causes can be various. So that headaches can be placed correctly, a thorough anamnesis (including the intake of painkillers, family history and coexisting symptoms), as well as a neurological and internist examination is necessary. There is a distinction between a primary and secondary headache. A tension headache is the most common type of primary headache. It usually results from stress or musculoskeletal disorders of the neck. Often the causes of headaches are also located in the area of the upper cervical spine (Atlas and Axis) and can be treated successfully. During physiotherapy, fasciae- and soft tissue techniques as well as manual therapy can help. In addition, the everyday posture (work and sleep) should be analyzed and a physiological position should be acquired by stretching and strengthening the muscles. To insure long lasting success, the patients receive relaxing- and personal exercises for home.
Functional disorders of the jaw joint
Disorders of the jaw joint can be various. Patients describe symptoms such as tensions in face and neck, grinding of teeth during the night, restricted opening or closing of the mouth, evasive movement while eating or also tinnitus. Aside of a dental or orthodontic treatment, a specific jaw joint therapy can ease discomfort. In this case, the muscles and joints of the jaw joint are mobilized and patients are guided through relaxation exercises. Additionally, neurological deficiencies, such as facial nerve paresis or a malfunctioning in the area of the Nerve trigeminus are part of the fields of treatment in jaw joint therapy.
Neck pain
Patients that sit during their tasks of employment know this type of pain well. By staying in this persistent, static position, the muscles start to tense up and pain and cramps are the result. Frequently pain in the neck can occur through a whiplash. If the pain stays local (does not radiate into the arms or head) and the pain does not appear at night, it usually is harmless. During therapy, treating the cause of discomfort should have a primary focus. The working posture is analyzed and optimally adopted to the environment, the cervical spine is examined for instabilities or restrictions of movement, shortened muscles are stretched and weakened muscles are strengthened.
Shoulder impingement
The shoulder is a band-, capsule- and muscle-secured joint. On the one hand, this provides a wide range of movement and on the other hand, it increases the risk of injury. Especially when working overhead or engaging in types of sports such as tennis, volleyball or swimming, the risk of impingement is increased. The impingement syndrome is an incarceration of the M. Supraspinatus tendon between the acromion and the shoulder head, where the lifting of the arm to the front or to the side is described as being very painful. This can also lead to a so-called calcified shoulder, where the inside of the affected tendon builds up calcium. For therapy it is firstly important that the tissue repair of the tendon is improved and secondly that the tissue receives enough space. This takes place by applying manual therapy and stabilizing motion exercises. Further important aspects of the impingement treatment are the straightening of the thoracic spine and the coordination training of the shoulder blade muscles.
Epicondylitis
Lateral epicondylitis, the so-called tennis elbow, is one of the most common musculoskeletal disorders of the working population and affects 40% of all people at one point in their life. The epicondylitis often develops through enduring strain during computer work or impact sports. In the most common cases, the muscle extensor carpi radialis brevis is affected. Mobilization, stretching and eccentric strengthening show good results within six weeks regarding pain and daily physical stresses. In addition, the mobilization of the cervical spine and the elbow joint are effective forms of therapy.
In case of lateral epicondylitis, an intensive physiotherapy should be performed. Surgery should only be considered when the symptoms persist for too long.
Low Back Pain
Back pain can have many different causes. Frequently, back pain is simply a functional disruption that does not stem from a serious pathology. This case is referred to as unspecific back pain. The cause of unspecific back pain often cannot be pinpointed precisely. Commonly the muscles, tendons or also joints cause the pain. Specific motion is essential for the treatment of unspecific back pain. Measured movement improves the muscle function, provides optimal provision of nutrients in the tissue and reduces the pain by releasing endogenous “medication”. Acute pain can be eased when manual therapeutic techniques, massages or heat applications are applied during physiotherapy.
However, if symptoms such as radiating pain, numbness or weakening of the arms or legs occur, worsening of coughing, sneezing, pressing or a night pain arises; a physician should be contacted straight away.
Unspecific low-back pain describes complaints that have arisen recently or suddenly or last for less than six weeks. In the most cases, acute back pain has a good prognosis with conservative therapy and subsides within a few weeks.
Herniated disc
A herniated disc occurs within the cervical spine as well as in the lumbar spine. Often the segments C5/6, L4/5 and L5/S1 are affected. The spinal disc protrusion and the disc prolapse can be distinguished. Herniated discs cause radiating pain (including abnormal sensations) in the arm or leg. The bending of the spine as well as coughing, sneezing or pressing worsen the symptoms. Surgery is usually only indicated if there is significant reduction of strength in addition to the other symptoms.
Conservative therapy prioritizes pain reduction through passive interventions (manual therapy, electrotherapy and muscle relaxation), improvement of agility, training of core stability and motion control as well as learning to move in way that protects your back.
Herniated discs must be diagnosed precisely by a medical professional – in this way you can improve your chances of a successful treatment.
Sympathetic Dysregulation
The vegetative nervous system is responsible for the unconscious and involuntary control of the body and therefore, for maintaining the inner balance. External factors such as stress, little sleep or also an unhealthy diet disturb our inner balance and can cause illness or functional disorders. By applying biofeedback, the vegetative status can be determined and the treatment can be adapted specifically. Possible therapeutic measures involve the training of breathing, active or passive relaxation techniques or manual mobilization of blockages. Aside of functional disorders, illnesses of the vegetative nervous system also exist. For instance, 2-5% of patients develop Morbus Sudeck (CRPS) after an injury of an extremity. Morbus Reynaud usually occurs during stress and reduces the blood circulation within the fingers suddenly.
Arthrosis
Arthrosis is an abrasion of the joint ligament. Over- as well as under-straining disturb the balance between cartilage build-up and cartilage degradation. This can lead to a degeneration of the cartilage substance. Run-in pain, pain due to exertion and restricted agility are the result. Cyclical- and motion exercises with a long duration over the entire range of motion are primarily indicated during therapy. To improve the restricted agility manual therapy techniques or fasciae treatments can be applied. The prognosis can be very different – while in many cases arthrosis slowly progresses, a rapid deterioration is also possible and a joint replacement therapy becomes unavoidable.
Arthrosis is an abrasion of joints. Today there are several different therapy options. A complete joint replacement is not necessary in every case.
Support is provided by Zunke Arthro Z3
Joint replacement therapy
If the arthrosis is so far advanced that the pain is unbearable, the joint replacement therapy (TEP) is the treatment of choice. Knee-, hip- and shoulder joints are regularly and very successfully replaced by artificial joints. In the acute phase, decongestant lymph drainages and pain-relieving techniques are used. During rehabilitation, the relearning of physiological movements and the full daily straining capacity is a primary focus. After optimal surgery and course of therapy, the patients can again carry out their daily and athletic activities.
Cruciate ligament and meniscus
Cruciate ligaments and menisci belong to the intraarticular structures of the knee joint. Both structures provide agility and guide the joint so that forces of cisaillement do not occur. They are essential for the optimal function of the joint. A typical mechanism of injury are high, jerky strains that directly affect the knee joint. Most of the cruciate ligament ruptures happen during skiing and playing soccer. During rehabilitation (postoperative and conservative), the current situation of the healing of tissue is determined through different tests. The therapy is then adapted accordingly so that the best-possible, muscular stability of the knee joint can be achieved.
The cruciate ligament tear is a common athletic injury. Usually the anterior cruciate ligament is affected. An important part of therapy is the strengthening and stabilizing of the muscles around the knee joint.

